Breast Cancer Clinic
Whether you’ve been referred by your doctor or want to self-refer to be safe, Mr Pieri offers breast cancer clinics to help you get the answers you need.
Discovering a change in the breast can be an extremely stressful event for a woman and her family. If you are concerned about a breast lump, breast pain, nipple discharge or any other change, then it is important to get this checked as soon as possible.
One Stop Breast Clinic
In our one-stop breast clinic, we offer a “triple assessment” in one day. First, you are assessed by Mr Pieri, a consultant specialist in breast cancer. He will establish whether you require a mammogram, an ultrasound or both.
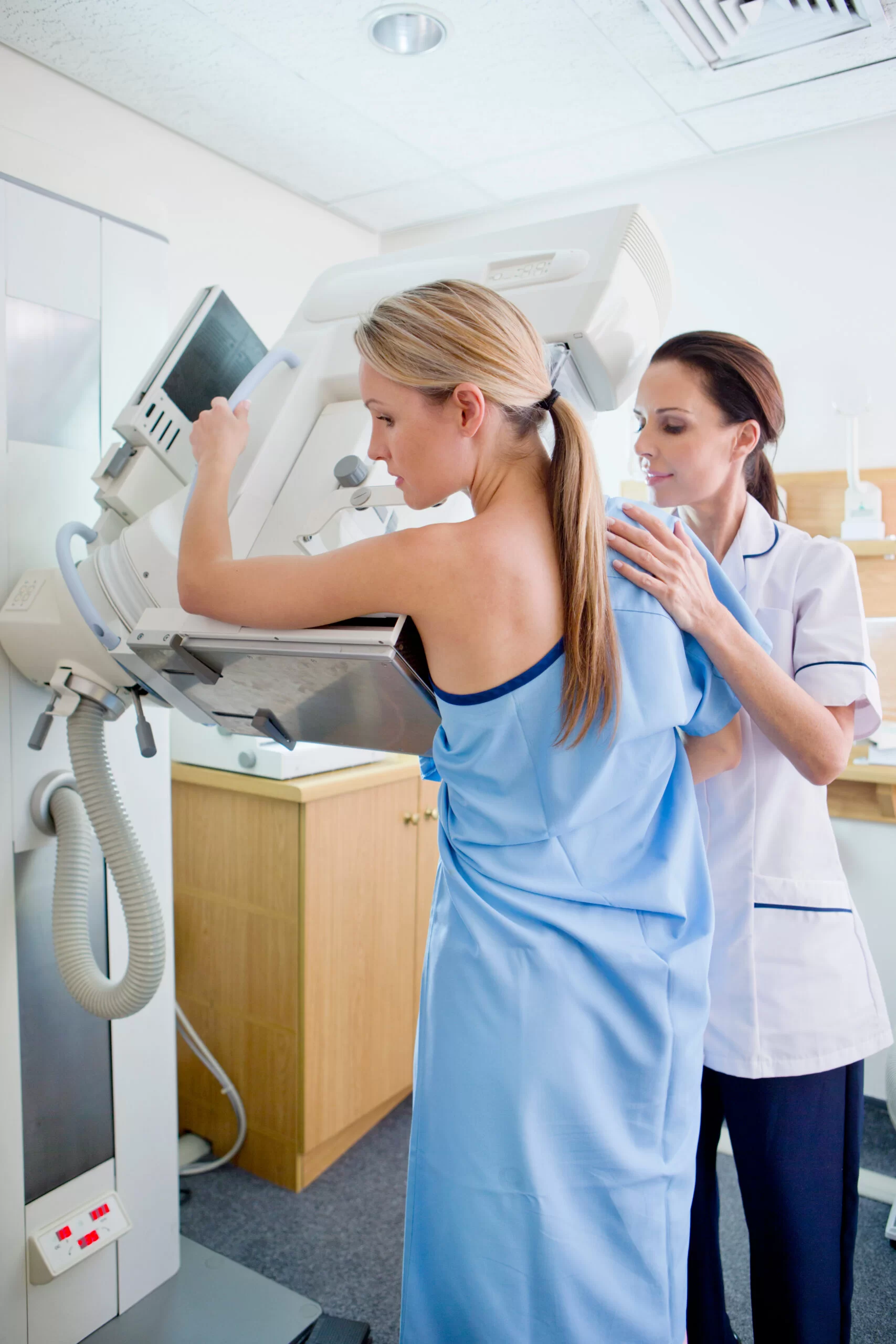
These breast scans will be carried out on the same day during one visit to the breast diagnostic clinic. If required, a breast tissue biopsy will also be performed. The scans and biopsies are carried out by a consultant specialist in breast radiology who works closely with Mr Pieri.
Research has shown that this “triple assessment” form of investigation is the best way to rule out breast cancer, with a 99.6% diagnostic accuracy.
Getting your breasts checked regularly can ensure we catch any potential health issues early. With the help of Mr Pieri, you can ensure you catch tumours before they spread and improve your chances of a smooth recovery.
Note: Currently, we cannot arrange a one-stop clinic appointment via our online booking portal. Please contact us for appointment information.
Breast Screening Frequently Asked Questions
Can I Self-Refer For A Private Mammogram?
Private mammograms can be self-referrals. So if your GP does not believe a referral is warranted due to your age or health, you’re unable to self-refer for NHS breast checks, or the waiting list is long, then you can use our private breast clinic to get the results you need quickly and efficiently.
What Happens During The Consultation?
When you arrive at the breast diagnostic clinic, Mr Pieri will review your medical history and examine your breasts. He will then decide whether you need a mammogram, ultrasound or both, and these will be carried out on the day of the appointment. A tissue biopsy may also be performed if required.
What Happens After The Consultation?
As mammograms and ultrasounds are outpatient procedures, you can leave on the same day. Mr Pieri will contact you and arrange a further appointment to discuss your results and any next steps required.
How Do I Book A Mammogram?
A mammogram is an X-ray technique used to check your breasts. It is just one of several types of breast diagnostic tools used to give you an accurate diagnosis. Booking a breast screening with Mr Pieri is incredibly easy: you can fill in the online form below or call +447526556934 to find out more information.

